We are about to hit the festive season, but it is also a time when many
people reflect on the past year and make plans for the next – including
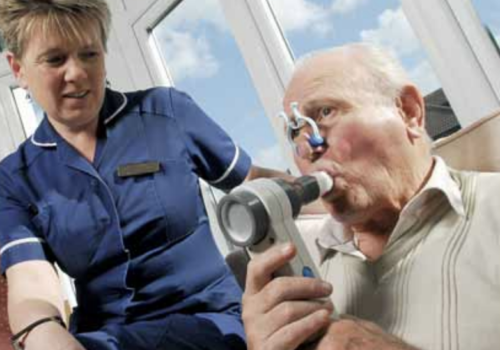
thinking about giving up smoking. In this issue we reflect on the impact of
the smoking ban in the UK. Hilary Wareing and Nina Gotz from the Tobacco
Control Collaborating Centre show how there have been significant benefits
in terms of air quality and increased numbers of quitters since the
smokefree legislation came into force between March 2006 and July 2007.
This has been a significant step forward in improving public health, and
provides a foundation to encourage more of your patients to quit.
The problem with asthma…
The current treatment of asthma in the UK is rightfully seen as a triumph of chronic disease management within a primary care setting. Almost all routine asthma care and, increasingly, elements of acute asthma care, are now provided in general practice. Over the past twenty years, significant effort and investment have gone into the production […]
Back to Basics: Anaphylaxis and adrenaline auto-injector pens
The Evaluation and Management of Cough in Adults
Cough as a symptom results in significant impairment of quality of life for patients. Its
wide and varied causes and presentations make diagnosis and management complex.
Many sets of guidelines have been produced to help clinicians in the evaluation and
management of acute and chronic cough. This article uses the British Thoracic Society
(2006) guidelines to provide a summary of the evaluation and management of cough.
Respiratory causes of breathlessness
The development of shortness of breath (SOB) is an expected outcome of overexertion,
as normally occurs after strenuous exercise. SOB occurring at rest or during marginal
exertion is considered abnormal. Multiple organ systems are involved in the differential
diagnosis of SOB but for the purpose of this article, we concentrate on the pulmonary
system and include chronic obstructive pulmonary disease (COPD), asthma, pneumonia,
pneumothorax, interstitial lung disease, lung cancer and dysfunctional breathlessness. This is
the second in a series of three articles focusing on diagnosis of the breathless patient.
How to write a business case
Skills in developing a business case may at first seem to be something far removed from
what a nurse would need. After all we are clinicians, we do the clinical things and
managers do things like business cases. How wrong could you be? This article shows
just how important business planning can be to both nurses and our patients.
Editorial: BJPCN End Of Year
As we reach the end of the year, BJPCN looks back at the challenges that
have been met in the care of patients with respiratory and allergic disease
over the past few years and looks forward to the new situations we will
have to face in the coming year. I have really enjoyed launching this
exciting journal and wish Monica Fletcher, Chief Executive of Education for Health, the very best as she takes on the editor’s role from the next issue.
Symbicort® (budesonide/formoterol) Maintenance and Reliever Therapy – Symbicort SMART® – A new approach to asthma management
Nurses know from first-hand experience that although asthma treatment has come a long way over the past few years, many patients with asthma remain uncontrolled. This results in unscheduled hospital appointments for patients and unnecessary limitations on their lifestyle.
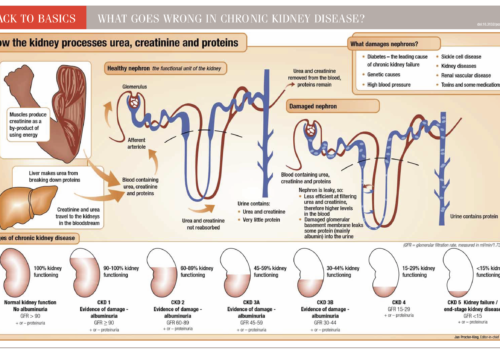
Making Sense of Chronic Kidney Disease (CKD)
What exactly is chronic kidney disease (CKD), what causes it and how is it diagnosed? In this article we get down to the basics of defining what CKD is, and explore the stages of CKD. We review CKD progression and the assessment and management recommendations for each stage of CKD.
Chronic Kidney Disease – Promoting Self-Management
This article will discuss the evidence for the self-management of long-term conditions, with a focus on chronic kidney disease (CKD). Self-management of CKD can include activities to control and manage blood pressure (BP); changes to diet such as reduced salt intake; smoking cessation; and understanding of the action and side-effects of prescribed medicines.