There are several different drug types used in the management of hypertension. This back to basics provides a useful summary of the different antihypertensive drug classes and how they act to regulate blood pressure.
This resource is fully searchable using the search box at the top of the page, or to narrow down your selection using filters click on 'Knowledge hub' in the main navigation.



People with COPD should be reviewed at least annually according to the Quality and Outcomes Framework. However, there is little mention of the importance of assessing nutritional status and no ‘QOF’ points for doing so. This article describes the assessment and management of COPD patients with a risk of malnutrition.
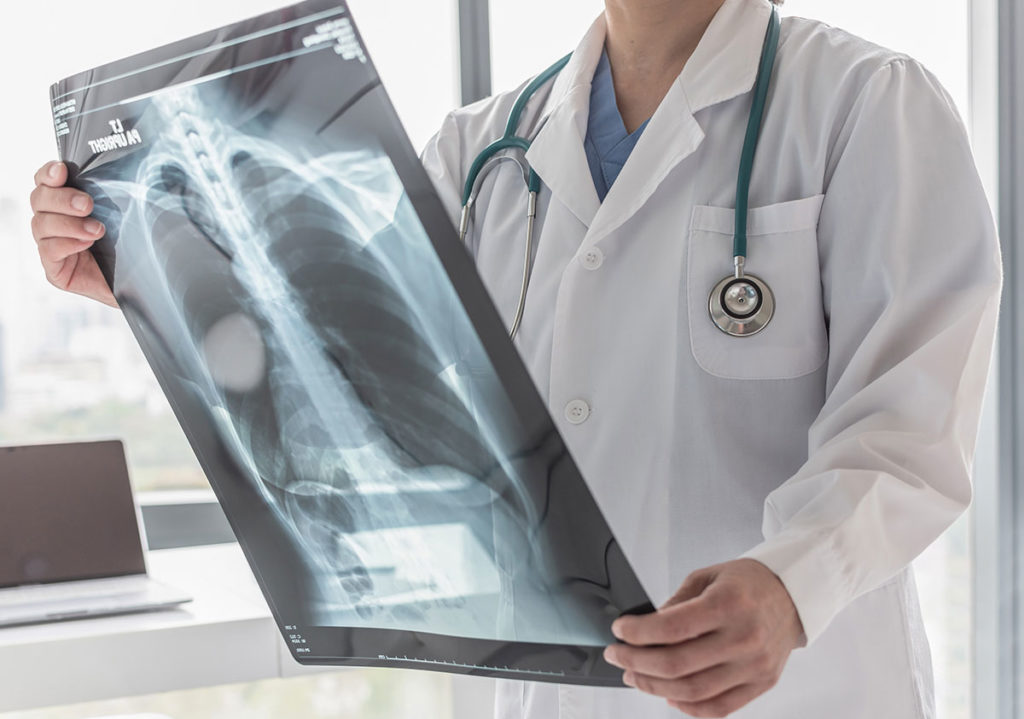
Heart failure is characterised by fatigue, breathlessness and retention of fluid. The update of the National Institute for Health and Clinical Excellence chronic heart failure guidelines has simplified its management by using a stepped approach to investigation and treatment. In this article, we focus on the practical aspects of managing the two main symptoms associated with heart failure – oedema and breathlessness.

Chronic obstructive pulmonary disease (COPD) is a largely preventable, slowly progressive, inflammatory disease. Rates of COPD are rising faster in women than in men, yet women are less likely to be diagnosed. There is currently no cure, but best-practice management outlined in recently updated NICE guidelines can help to improve patients’ symptoms and quality of life.

Chronic clinical conditions have traditionally been regarded as individual disease categories within individual patients, although there is often considerable overlap across clinical systems. However, for those managing these patients the presence of various co-morbidities is all-too apparent. It may be time to consider a new approach to management of these patients.
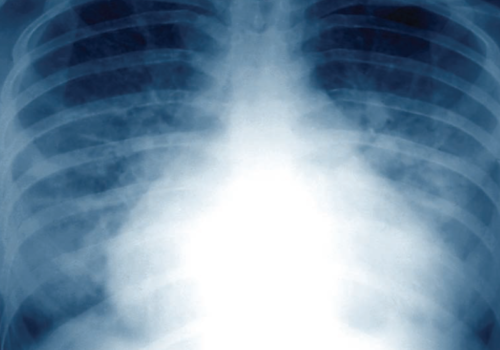
Cardiovascular morbidity and mortality in patients with chronic obstructive pulmonary disease (COPD) is nearly double the rate in the general population without COPD. And for those with cardiovascular disease (CVD) and COPD, heart failure is the most common cause of hospitalisation.
Chronic clinical conditions have traditionally been regarded as individual disease categories within individual patients, although there is often considerable overlap across clinical systems. The monitoring of patients with long-term conditions has historically centred around a traditional model of a nurse-led clinic, utilising an appropriate level of skill mix. The disease categories and associated clinical indicators of the Quality and Outcomes Framework (QOF) have encouraged this approach, but for those managing these patients the presence of various co-morbidities is all too apparent
Acute exacerbations of chronic obstructive pulmonary disease (COPD) are common and
have serious implications. They greatly reduce patients’ quality of life and often result
in hospital admissions. Acute exacerbations of COPD are the largest single cause of
emergency respiratory admissions and each exacerbation results in an average hospital
stay of 10.3 days. In this article we review what causes exacerbations in patients with COPD and
how you can help to prevent and treat them effectively.

On 23 June 2005, the Met Office issued a warning that severe thunderstorms were likely
to hit the South East of England in the next 24 hours. On the evening of Friday 24 June,
primary care out-of-hours services and hospital accident and emergency departments
in Northwest London were inundated by patients attending with acute asthma. The
scale of these attendances – eight times more patients than usual in one hospital – meant that
departments had to call in additional staff and some ran out of emergency supplies of
bronchodilators, nebulisers and oral steroids for treating asthma. In this article, we will explain
the background and some of the theories related to this type of epidemic of acute asthma –
Thunderstorm Asthma.
A unique new e-platform for primary care

For healthcare professionals in countries with applicable health authority product registrations. The content may not be approved for use in your specific region or country. Please review the applicable product labelling for your country for indications and instructions prior to use. If not approved, please exit this site.
We use cookies to ensure that we give you the best experience on our website.
By continuing to this site you are confirming that you are a healthcare professional and are opting into the use of cookies.


















