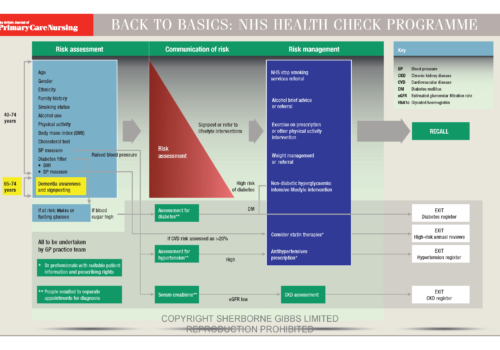
In general, deaths from cardiovascular disease (CVD) are falling, except for the forgotten CVD, dementia. The rate of dementia is rising year on year and it is now one of the top 5 causes of death in the UK. Risk factors for dementia are similar to other CVDs and risk modification can reduce the risk of development of the condition.