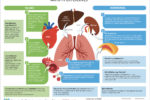
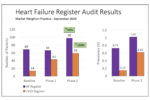
The British Heart Foundation is pressing for a renewed focus on improving the diagnosis and management of familial hypercholesterolaemia, and adoption of a nationwide cascade screening programme for first-degree relatives. The article includes best practice tips for busy primary healthcare professionals.