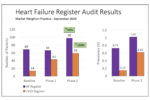
The outlook is bleak for patients with untreated or suboptimally treated heart failure (HF). Conversely, optimising management (HF) improves patient survival and reduces hospital admissions. However, standards of care continue to vary, and many HF patients are still not receiving recommended therapy with disease-modifying drugs or specialist input to their care. Outcomes will only improve for all our HF patients if evidence-based clinical guidelines are implemented throughout the NHS.