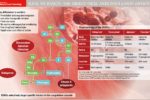
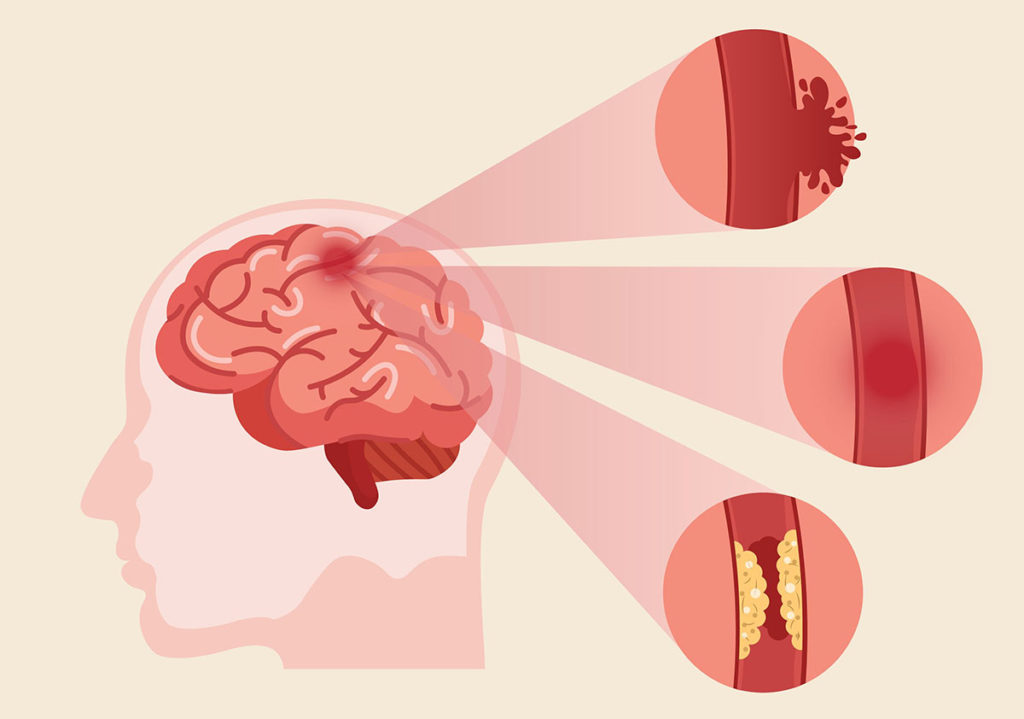
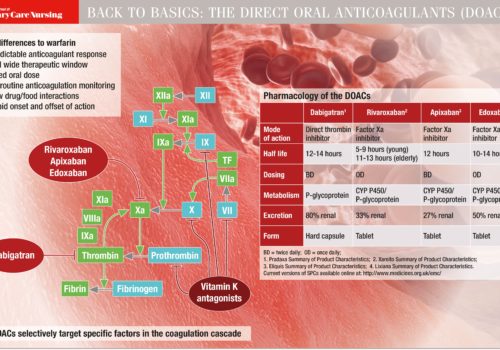
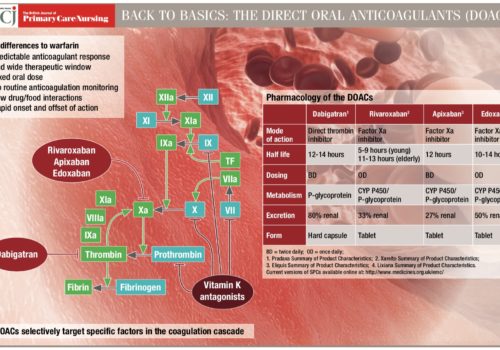
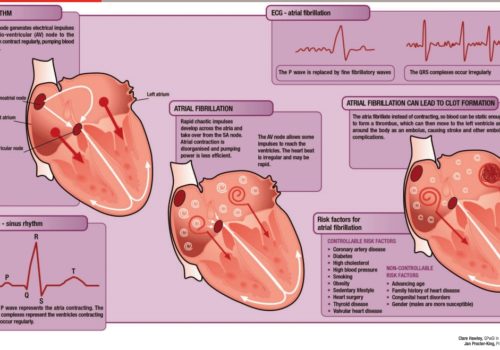
Since 2014 the 15 Academic Health Science Networks (AHSNs) across England have been working on a collaborative atrial fibrillation (AF) programme focused on reducing AF-related stroke. The national programme has three elements: Detect: finding more people with AF to allow early intervention to prevent stroke; Protect: treating more at-risk patients with anticoagulants to reduce the rate of AF-related stroke; and Perfect: improving the quality of anticoagulation to ensure maximal patient outcomes.