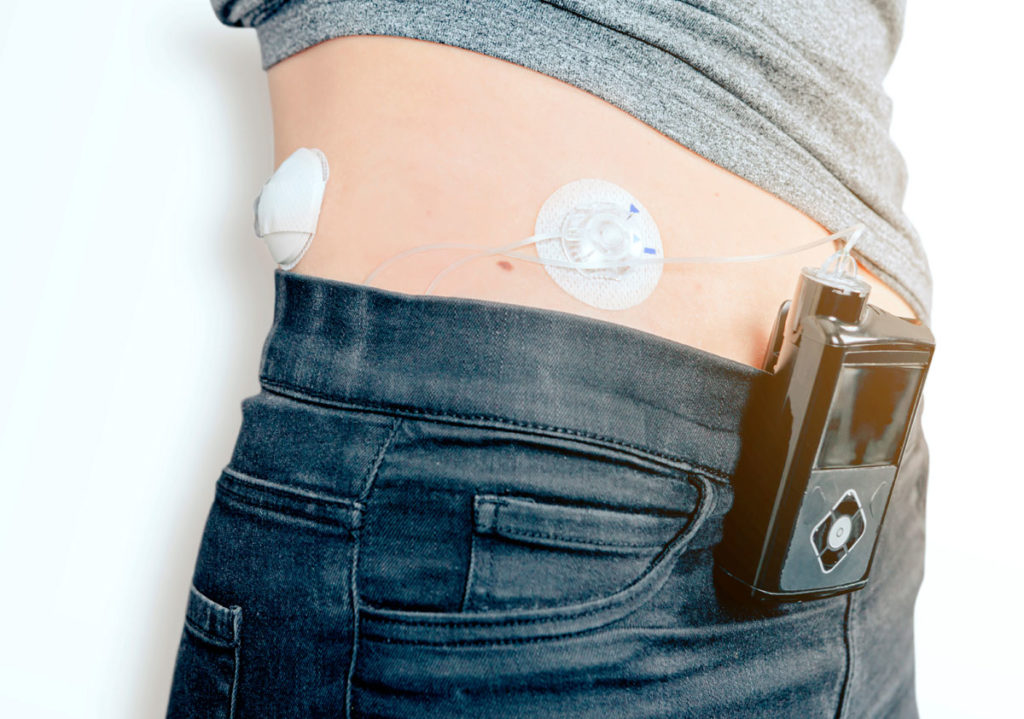
Patients with chronic conditions such as heart disease or diabetes need to plan carefully before travelling long distances and taking holidays. Lifestyle changes can have an important impact on disease control, but a bit of thought and preparation beforehand should ensure that your patients’ holidays are both happy and healthy.