Volume 7, Supplement 2, Jul-Aug-Sep 2010


This resource is fully searchable using the search box at the top of the page, or to narrow down your selection using filters click on 'Knowledge hub' in the main navigation.



More than 4.9 million people in the UK have diagnosed diabetes and by 2030 Diabetes UK estimate there will be 5.5 million people with diabetes.
The care of patients with diabetes – particularly type 2 diabetes which counts for about 90% of patients seen in primary care – is a significant challenge.
Our resources focus on:
![]() Detection of pre-diabetes conditions frequently associated with obesity and metabolic disorders
Detection of pre-diabetes conditions frequently associated with obesity and metabolic disorders
![]() Early diagnosis of type 2 diabetes
Early diagnosis of type 2 diabetes
![]() Interventions to reduce the risks of cardiovascular and renal disease (the cardio-renal syndrome)
Interventions to reduce the risks of cardiovascular and renal disease (the cardio-renal syndrome)
![]() Glycaemic control with established therapies including metformin
Glycaemic control with established therapies including metformin
![]() The roles for newer agents including SGLT2 inhibitors and DDP-4 inhibitors
The roles for newer agents including SGLT2 inhibitors and DDP-4 inhibitors
![]() Importance of lipid (cholesterol) management and antihypertensive therapy
Importance of lipid (cholesterol) management and antihypertensive therapy
Additional contributions discuss:
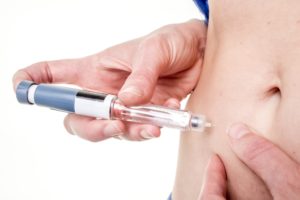
![]() The initiation and intensification of insulin in people with type 2 diabetes
The initiation and intensification of insulin in people with type 2 diabetes
![]() Diagnosis and management of people with type 1 diabetes
Diagnosis and management of people with type 1 diabetes
![]() Prevention of hypoglycaemia
Prevention of hypoglycaemia
Diabetes clinics form a major part of the workload for practice nurses, but 95% of routine diabetes care is delivered by patients themselves or by family members and carers. It is imperative that we offer people with diabetes concise, up-to-date education for effective foot care and to prevent complications.
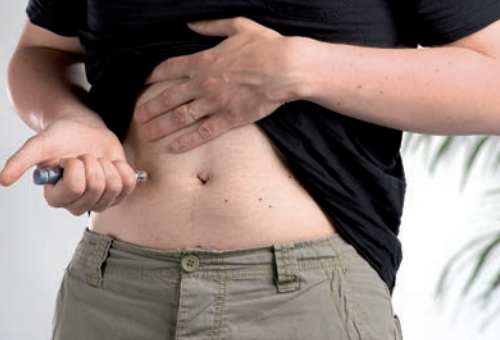
In the UK, an estimated 1 million people with diabetes use injectable therapies, and these patients are increasingly being managed in primary care. As a result, more primary care nurses are taking responsibility for the initiation and continuing management of injectable therapies, including advising on and reviewing an individual patient’s injection technique.
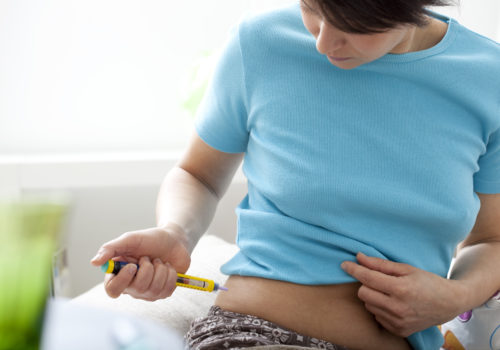
Insulin therapy is life-saving for people with type 1 diabetes, and a key component of the treatment regimen for many people with type 2 diabetes. At the same time, insulin is a major cause of adverse drug events, some of which are so severe that they cause emergency admission to hospital. There is therefore much that needs to be done to improve the safe use of insulin in order to reduce medication errors and hospitalisation associated with hypoglycaemia.
Erectile dysfunction (ED) is three to four times more common in men with diabetes, and 20% have the condition at diagnosis. ED is a marker for heart disease, and men themselves value the opportunity to discuss their sexual problems with a health professional. The annual diabetes review offers the opportunity to identify and treat these men. Some practice nurses may find this task daunting, but treatment of ED can help to improve a man’s wellbeing and reduce his cardiovascular risk.
In this paper, we summarise previously reported findings from the MY-WAIST study, which aimed to evaluate a primary care strategy for identifying people with undiagnosed type 2 diabetes or at increased risk of developing this condition. Recruitment was unexpectedly low, but the qualitative data collected, including interviews with healthcare providers, helped to highlight some of the reasons for poor uptake of the appointments offered. Perceived barriers to recruitment included heavy workloads and competing demands in primary care. Lower uptake in people from harder-to-reach groups was identified in our quantitative findings and was also suggested by healthcare providers’ perceptions about the characteristics of patients who attended.
Successful management of individuals with diabetes, or any other single component of the metabolic syndrome, requires treatment of all the related physiological systems as a whole. This treatment must be underpinned by the management of obesity, and drugs should be preferred that address the entire portfolio of the metabolic syndrome.

NICE recommends that all patients with diabetes should be offered a structured educational programme at diagnosis, together with regular reviews and updates. Several programmes are available that meet NICE criteria, and there is evidence that they can help to improve patients’ quality of life, well-being and diabetic control.
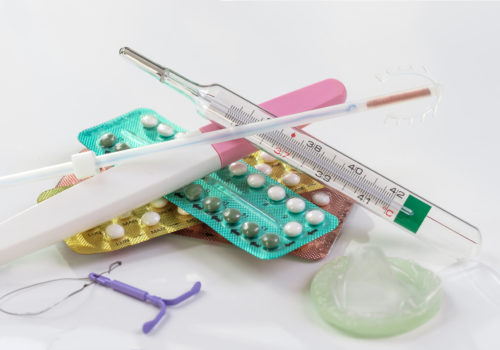
Unplanned pregnancy with poor glycaemic control at conception is associated with major maternal and perinatal complications. However, contraception is used haphazardly by women with diabetes and is often not discussed by diabetes professionals. GPs and practice nurses need to be able to give appropriate advice about contraception to the increasing numbers of women of childbearing age with type 1 and type 2 diabetes.
There are now four agents in the new class of glucose-lowering agents called dipeptidyl peptidase-4 inhibitors (DPP-4 inhibitors) available in the UK. They are, in order of launch in the UK, sitagliptin, vildagliptin, saxagliptin and linagliptin. Several others are in the pipeline and are likely to be launched before long. This article will discuss their place in treating diabetes and the differences between them.
Dapagliflozin (Forxiga) is the first in a new class of oral antidiabetic drug that has been given the go-ahead for marketing in Europe, including the UK. Described as a sodium glucose cotransporter 2 (SGLT2) inhibitor, this new preparation works on the kidneys to lower blood glucose. What does this new drug have to offer and how can it potentially help our patients with type 2 diabetes?
A unique new e-platform for primary care

For healthcare professionals in countries with applicable health authority product registrations. The content may not be approved for use in your specific region or country. Please review the applicable product labelling for your country for indications and instructions prior to use. If not approved, please exit this site.
We use cookies to ensure that we give you the best experience on our website.
By continuing to this site you are confirming that you are a healthcare professional and are opting into the use of cookies.


















