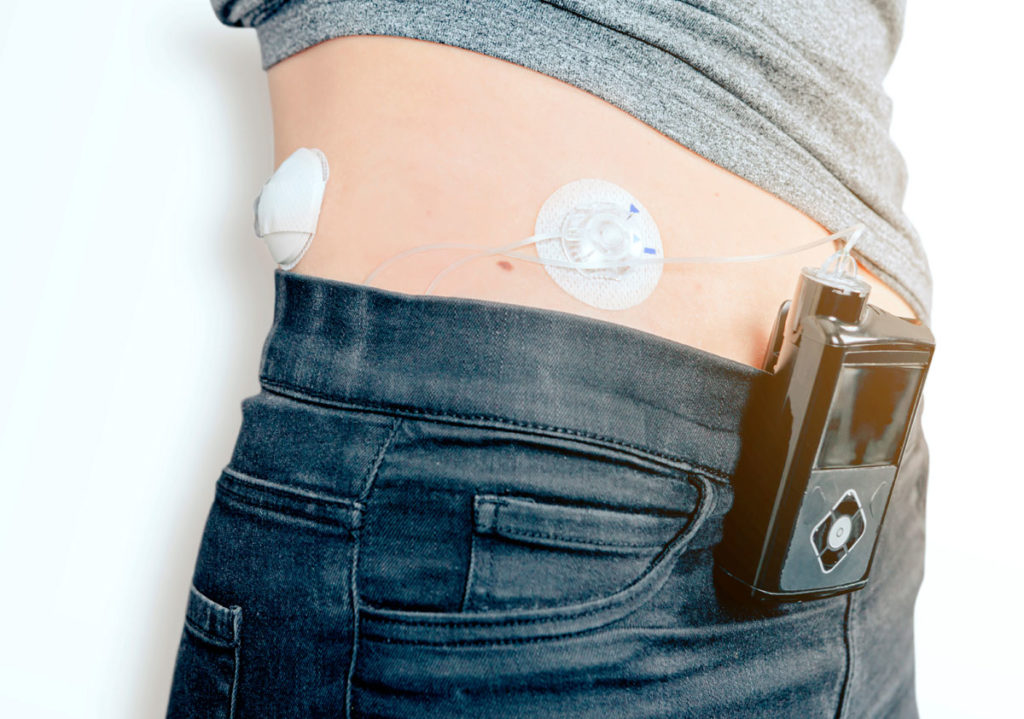
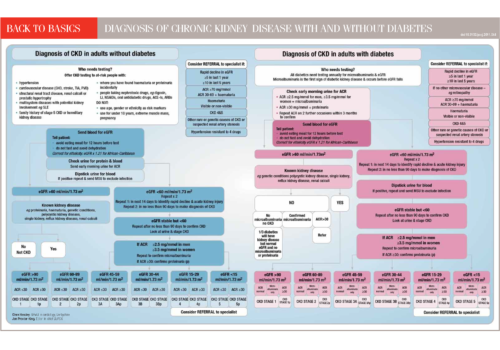
The National Institute for Health and Clinical Excellence (NICE) recommends that all people with diabetes should receive nine key tests at their annual diabetes review. These important markers ensure diabetes is well controlled and are designed to prevent longterm complications. The nine key tests are: weight, blood pressure, smoking status, HbA1c, urinary albumin, serum creatinine, cholesterol, eye examinations and foot examinations. This review discusses the importance of each marker of improved long-term care of patients.